 2810 N Church St, Ste 67778, Wilmington, DE 19802-4447
2810 N Church St, Ste 67778, Wilmington, DE 19802-4447 Toll Free: (877) 466-3366
Toll Free: (877) 466-3366Core xRM is now ConnectHealth. Learn more about our name change here.
 2810 N Church St, Ste 67778, Wilmington, DE 19802-4447
2810 N Church St, Ste 67778, Wilmington, DE 19802-4447 Toll Free: (877) 466-3366
Toll Free: (877) 466-3366Core xRM is now ConnectHealth. Learn more about our name change here.
The Provider Data Quality (PDQ) solution utilizes a blend of technology and stringent policies to definitively verify existing provider directory data at the source. It provides flexibility to provider groups for easy and efficient response to ensure state and federal provider data requirements are met quarterly. The proven processes achieve high level of engagement from providers resulting in the highest levels of data accuracy.
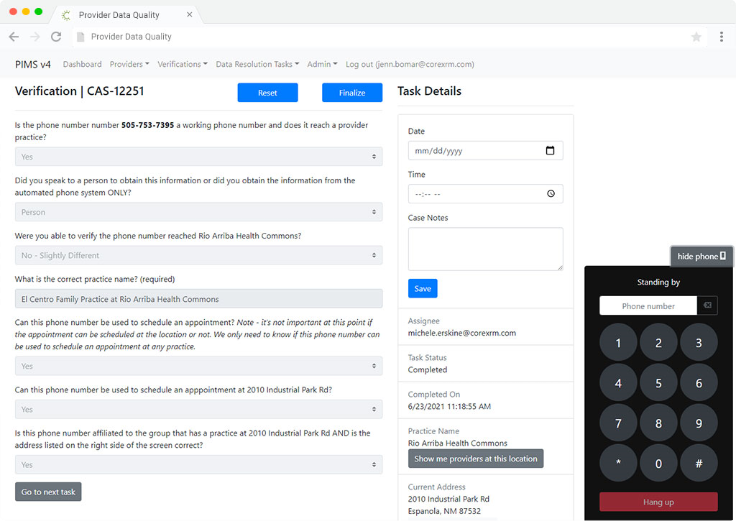

Arm provider data stakeholders with a definitive assessment and recommended actions to the existing provider data set. Competitors utilize data aggregation to provide a confidence score on your data which leaves business owners questioning if the new information should be implemented. Our approach is definitive. We dial phone numbers, speak to provider groups, and follow up to ensure quarterly deadlines are met in providing attestation of all information gathered.

Offering provider groups multiple methods for reviewing, maintaining, and updating their data dramatically improves provider engagement. Whether selecting the online portal, fax, or telephone-based verification option, providers experience a highly efficient verification process. This provider participation is key in ensuring your provider directory stays up to date.
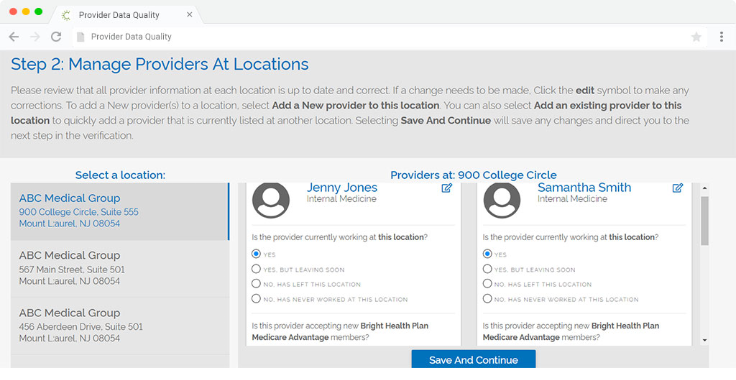
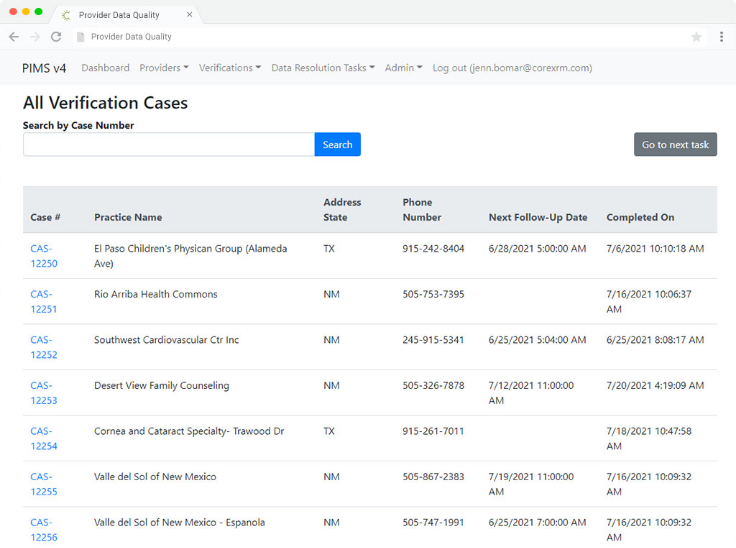

An audit adds strain to any company. With the Provider Data Quality solution providing an audit trail is simple. The solution provides access to all the details and attestations needed to prove you have collected accurate information. The solution has been utilized by industry leaders to successfully pass their state and federal audits.

The Provider Data Quality solution has already been successful in helping industry leaders through state and federal audits.

Providers have given highly positive feedback on how easy it is to update their information via the web portal.

The PDQ solution can be branded to ensure providers know who is asking for their updated information.
